Syphilis is a sexually transmitted disease (STD) caused by the spirochete bacterium - Treponema pallidum (T. pallidum) which can be spread by sexual contact, by blood transfusion, and via vertical transmission. Syphilis affects 12 million people worldwide annually and results in significant morbidity if not mortality.
According to NACO, in 2011, incidence of Syphilis had reduced to about 1% in India. However, recent studies indicate a rise in the prevalence of Syphilis in the country. Among blood donors in India it was recently reported to be 0.7%. Though the cases of primary syphilis have declined, there has been a concomitant rise in secondary and early latent syphilis.
Syphilis is a complex, acute or chronic infectious disease with diverse clinical manifestations, depending upon the stage of infection and the individual response. The disease progresses through distinct primary, secondary, latent and tertiary stages. The ulcers that appear in primary and secondary syphilis are rich in treponemes; venereal transmission occurs through direct contact with these lesions. The period of incubation ranges from 10 days to 3 months and antibodies are usually detected after 2-4 weeks from the primary lesion.
Screening of blood for syphilis is mandatory for issuing safe blood. Antibodies to syphilis infection become detectable 3 to 4 weeks after exposure and may remain detectable for long periods after the treatment. Two group of antibodies are formed viz. one reactive with the non-Treponemal antigen used and other reacting with specific antigens of Treponema pallidum. Antibody to non-Treponemal antigens is found in active disease and the levels subside after successful treatment, while Treponema-specific antibodies persist for a long time after the infection has been successfully treated.
The serological tests most commonly used to screen for the disease are the non-Treponemal and Treponemal tests. The non-Treponemal tests such as RPR or the VDRL tests, measure the host’s response to non-Treponemal antigens such as cardiolipin and lecithin released from the damaged host cells, as well as lipoprotein-like material released from the Treponema. Non-treponemal tests become positive shortly after initial infection, peak during the secondary or early latent stage, and then decline with time. Hence, their disadvantages are false-positive reactions, due to the prozone phenomenon and lack of sensitivity in the late stage of infection.
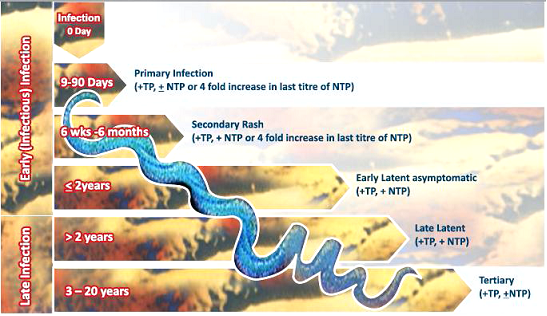
Spirochetes may remain alive and continue to replicate in immunologically sequestered sites in the body even with a brisk initial immune response and no outward clinical manifestations of disease in at least 1 of 4 persons who are not treated. In late latent syphilis, after many years of latency, treponemes begin to multiply leading to recurrence. Hence, Treponemal tests are used as diagnostic tests in patients with nonreactive non-treponemal tests but with signs and symptoms of late syphilis. Treponemal tests are also used mainly as confirmatory tests to verify reactivity in non-treponemal tests as they have been proven to have high sensitivity for all the stages of disease other than very early primary syphilis.
Besides higher sensitivity and specificity, the advantages of ELISAs are the capacity to process large number of samples and ability to have a print out of the objective spectrophotometric readings.
Keeping the pace with the recent advances in the field of Syphilis diagnosis, Transasia Bio-Medicals Ltd. offers ErbaLisa Syphilis ELISA, a third generation Treponemal test, based on the sandwich method, for advanced Treponemal screening. It uses a mixture of recombinant Treponemal antigens, TpN15, TpN17 and TpN47, for the detection of total antibodies (IgG, IgM, IgA) against Treponema pallidum in human serum/plasma, and therefore, is useful in the diagnosis of Syphilis at all the stages.
References:
- http://www.antimicrobe.org
- The Laboratory Diagnosis of Syphilis. Sam Ratnam. Canadian Journal of Infectious Diseases and Medical Microbiology. 2005 Jan-Feb; 16(1): 45–51.
- Comparative study of Treponemal and non-Treponemal test for screening of blood donated at a blood center. Narinder Kaur Naidu, Z. S. Bharucha, Vandana Sonawane, and Imran Ahmed. Asian Journal of Transfusion Science. 2012 Jan-Jun; 6(1): 32–35.